Article Highlights
Perceived risk of COVID-19 infection was found to be inversely related to sleep quality.
Sense of meaning in life mediated the relationship between perceived risk of COVID-19 infection and sleep quality.
Low perceived social support exacerbated the association of perceived risk of COVID-19 infection with sense of meaning in life.
To improve sleep during public health crises, public health interventions should address both social support and sense of meaning in life.
The COVID-19 pandemic that emerged in late 2019 has dramatically underscored the profound health, social, and psychological disruptions that infectious diseases cause. The immediate effects of the pandemic have been widely documented, but the broader implications—specifically, the influence of infection-related fears on mental and physical well-being during global health crises—remain less thoroughly examined. In this study we took the COVID-19 pandemic as a case to explore the mechanisms through which perceived risk of infection affected sleep quality during the pandemic, thereby expanding the cognitive framework for understanding the psychological mechanisms of sleep disturbances in health crises. By doing so, we aimed to contribute to a universal theoretical foundation for understanding the deeper psychological pathways that contribute to impaired sleep health during public health crises.
Public health crises often lead to widespread psychological distress, resulting in increased anxiety, depression, and stress (Lu et al., 2024; Wolfson et al., 2021). During the COVID-19 pandemic, populations worldwide experienced coronasomnia (a portmanteau of “coronavirus” and “insomnia”; S. Chen & Cheng, 2024; Cheung et al., 2024), caused by multiple stressors related to infection fear, social isolation, and disrupted life rhythms (S. Chen & Cheng, 2024). However, although some evidence in existing research has supported a direct link between pandemic-related stress and sleep disorders (Jahrami et al., 2021), other studies found no significant associations between these variables (e.g., Gao & Scullin, 2020). This discrepancy underscores the importance of further exploring the diverse mechanisms underlying sleep disturbances during public health crises, with a particular focus on the role of moderating factors, such as social support (Fu et al., 2022; Gruenewald et al., 2020).
Using cognitive appraisal theory (Folkman et al., 1986) and the strong situation hypothesis (Cooper & Withey, 2009) as a basis, we examined how the perceived risk of infection influences sleep quality, with a focus on the mediating role of a sense of meaning in life and the moderating effect of perceived social support. Perceived risk is a key psychological stressor during pandemics, and has been shown to exert a significant influence on mental and physical health outcomes (C. Liu et al., 2021; Svenson et al., 2024). Empirical evidence has consistently demonstrated that COVID-19 risk perception directly impairs sleep quality through heightened vigilance and anxiety responses. Notably, Lin and Chung’s (2021) longitudinal study of 1,482 adults during lockdowns found that each point of increase on the COVID-19 Risk Perception Scale predicted 18% greater odds of clinical insomnia, mediated by worry-related arousal. This aligns with the finding by Zerbini et al. (2022) that pandemic-related sleep disruptions were predicted by subjective risk appraisal. It has been found that a perceived risk exceeding 30% above baseline levels triggers clinically significant anxiety and emotional distress, which, in turn, disrupts sleep architecture through both cognitive hyperarousal and physiological stress responses (Alimoradi et al., 2022; Huang et al., 2024). The strong situation hypothesis (Cooper & Withey, 2009) suggests that external stressors, such as those that pandemics create, can intensify the effects of the individual’s perception of risk on psychological outcomes, including sleep disturbances (I.-M. Chen et al., 2024; Wismans et al., 2022). Accordingly, we proposed the following hypothesis:
Hypothesis 1: Perceived risk of COVID-19 infection will directly predict poor sleep quality.
Meaning in life, which refers to a sense of purpose and coherence in one’s existence (Steger et al., 2009), exhibits the characteristic of a double-edged sword in the context of a public health crisis. On one hand, a strong sense of meaning in life can buffer the effects of uncertainty and reduce the transmission of anxiety to sleep quality (Brown & Papp, 2024; Martins et al., 2022); on the other hand, acute threat perceptions (e.g., perceived infection risk) may deplete cognitive resources, undermining the meaning system (Shechter et al., 2020). Furthermore, prolonged exposure to a crisis event could trigger meaning reconstruction motivation (Krok & Zarzycka, 2020). This duality aligns with Park’s (2010) meaning regulation theory, in which it is posited that meaning systems can both stabilize and destabilize depending on contextual demands (e.g., acute vs. chronic crises). In the context of pandemic fluctuations, when individuals can effectively integrate risk perception with a sense of meaning in life, this may mitigate the negative impact on sleep quality; conversely, viewing the risk as a threat would enhance its negative effects on sleep quality (I.-M. Chen et al., 2024). Therefore, we proposed the following hypothesis:
Hypothesis 2: Sense of meaning in life will partially mediate the relationship between perceived risk of infection and poor sleep quality.
Perceived social support—defined as the belief in the availability of supportive relationships (Hupcey, 1998)—is another factor that is critical in understanding the connections among perceived infection risk, sense of meaning in life, and sleep quality. Adequate social support can help individuals to maintain the stability of their meaning system during stressful situations by enhancing psychological resilience (Feeney & Collins, 2015). For example, Fu et al. (2022) demonstrated that perceived social support moderates the relationship between psychological states (e.g., awe) and prosocial behaviors by reinforcing a sense of meaning in life. In the pandemic context, perceived social support may buffer the negative effect of perceived risk of infection on sense of meaning in life, thus indirectly protecting sleep quality. As such, we formed the following hypothesis:
Hypothesis 3: Perceived social support will moderate the indirect effect of perceived risk of infection on poor sleep quality through sense of meaning in life, such that this effect becomes weaker among individuals with stronger social support.
Our research model is shown in Figure 1. By positioning the findings within the broader context of pandemic-related stress, this research will contribute to a more generalizable understanding of the psychological and social factors that influence sleep health during a global health crisis. Furthermore, the insights gained from this study will have practical implications for the design of interventions aimed at promoting mental health and well-being during health emergencies.
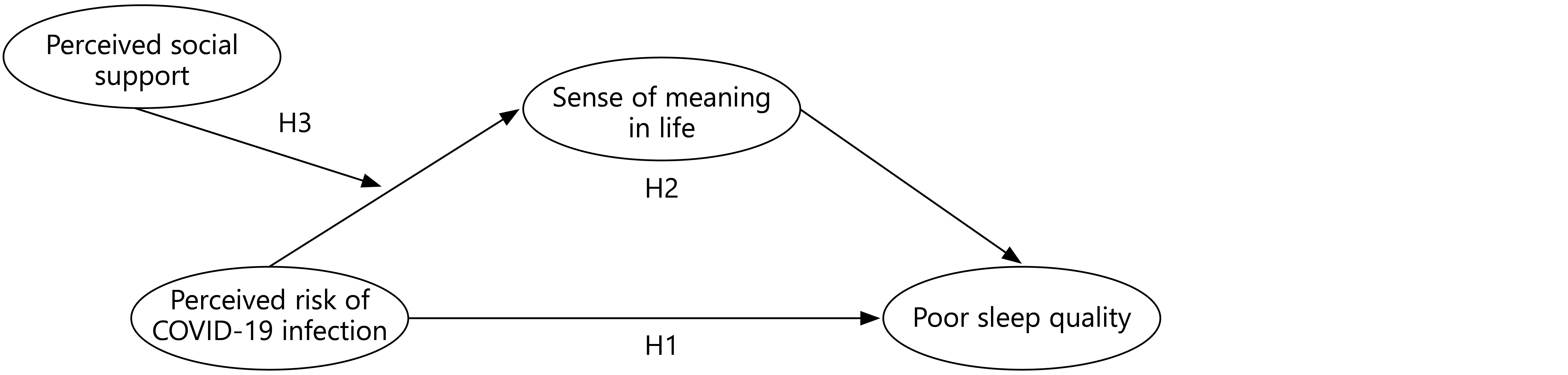
Figure 1. Theoretical Research Model
Method
Participants and Procedure
This research was approved by the Scientific Review Committee of the Neuroeconomics Laboratory at Guangzhou Huashang College and conformed with the ethical principles of the Declaration of Helsinki. All respondents were informed that the survey data would be used for research purposes only, and that their participation was voluntary and entirely anonymous, except for certain demographic data.
The requisite sample size was estimated using G*Power 3.1 (Faul et al., 2007), with an effect size of .25 and alpha set at .05, requiring a minimum of 159 participants. Between October 28 and November 21, 2022, we randomly recruited 486 Chinese participants online via
www.sojump.com, a large survey platform similar to MTurk in the United States. Automatic screening of internet protocol addresses was performed on the platform to ensure that each survey was completed only once. We excluded responses if the completion time for the survey was less than 2 minutes or exceeded 30 minutes, with time limits determined based on the length and content of the survey. After removing 35 incomplete or invalid responses, the final sample consisted of 451 participants, of whom 53.82% (
n = 243) were women and 46.18% (
n = 208) were men. The age distribution was as follows: 34 (7.54%) were aged under 20 years, 151 (33.48%) were aged 20–29 years, 128 (28.38%) were aged 30–39 years, 82 (18.18%) were aged 40–49 years, 44 (9.76%) were aged 50–59 years, and 12 (2.66%) were aged 60 years or over. To control for order effects, the presentation of scales was randomized. To enhance data quality, respondents each received compensation of RMB 3 (USD 0.50).
Measures
Perceived risk of COVID-19 infection was measured using three items (e.g., “I feel that the current situation of the pandemic is very serious”) adopted from Zhang et al. (2022), with responses recorded on a 5-point Likert scale ranging from 1 (completely disagree) to 5 (completely agree), such that higher scores indicate greater perceived risk. In this study Cronbach’s alpha was .73.
Sleep quality was assessed using the Pittsburgh Sleep Quality Index (Buysse et al., 1989), which was translated into Chinese by X. Liu et al. (1996). This 19-item measure is designed to evaluate sleep quality over the past month across seven components: (a) subjective sleep quality (one item: “How would you rate your sleep quality overall?”), (b) sleep latency (two items, e.g., “How often did it take you more than 30 minutes to fall asleep?”), (c) sleep duration (one item, assessed by actual hours slept per night), (d) habitual sleep efficiency (three items, calculated as the ratio of time asleep to time spent in bed), (e) sleep disturbances (nine items, e.g., “How often did you wake up in the middle of the night?”), (f) use of sleep medication (one item, based on frequency of medication use for sleep), and (g) daytime dysfunction (two items, e.g., “How often did you have trouble staying awake during daytime activities?”). Each component is scored from 0 to 3 using distinct operationalizations. For subjective ratings (e.g., sleep quality) Likert-type scales are used, ranging from 0 (very good) to 3 (very bad). Frequency-based items (e.g., sleep medication use) are scored as 0 (not during the past month), 1 (less than once a week), 2 (once or twice a week), and 3 (three or more times a week). Quantitative measures such as sleep duration are categorized into four tiers: 0 = ≥ 7 hours, 1 = 6–7 hours, 2 = 5–6 hours, and 3 = < 5 hours. The total score ranges from 0 to 21, with higher scores indicating poorer sleep quality. In this study Cronbach’s alpha was .77.
Social support was measured using the Multidimensional Scale of Perceived Social Support (Zimet et al., 1988), which was translated into Chinese by Wang et al. (2017). This 12-item scale is designed to assess perceived support from friends, family, and significant others (e.g., “I have friends with whom I can share joys and sorrows”). Items are rated on a 7-point Likert scale ranging from 1 (very strongly disagree) to 7 (very strongly agree), with higher scores reflecting greater perceived support. Cronbach’s alpha in this study was .90.
Perceived meaning in life was measured with the Scale of Meaning in Life, which was designed by Steger et al. (2006) and translated into Chinese by S. Liu and Gan (2010). It contains 10 items, five of which are allocated to each of the two subdimensions: searching for meaning in life (e.g., “I am always looking to find my life’s purpose”) and presence of meaning in life (e.g., “I understand my life’s meaning”). Participants answer the items using a 7-point Likert scale ranging from 1 (completely disagree) to 7 (completely agree), and higher total scores indicate a stronger sense of meaning in life. In this study Cronbach’s alpha was .85.
Data Analysis
We tested the moderated mediation model in this study using SPSS 22.0. A partial correlation analysis was performed to examine relationships among the study variables while controlling for gender and age. Next, we used Model 7 of the PROCESS macro (Hayes, 2018) to examine the moderated mediation model, with perceived risk as the independent variable, sense of meaning in life as the mediator, perceived social support as the moderator, and sleep quality as the dependent variable. All variables were standardized, and gender and age were included as covariates. We employed the bootstrapping method (Hayes & Scharkow, 2013) with 5,000 resamples and 95% bias-corrected confidence intervals (CIs) to test the significance of indirect effects while controlling for covariates. Indirect effects were considered significant if the 95% CI excluded zero.
Results
Table 1 presents the descriptive statistics and bivariate correlations among study variables. Data normality was confirmed using skewness and kurtosis, with values within acceptable limits (skewness < 2, kurtosis < 7; West et al., 1995). Pearson correlations showed that the perceived risk of COVID-19 infection was positively associated with sense of meaning in life, perceived social support, and poor sleep quality. Both sense of meaning in life and perceived social support were negatively correlated with poor sleep quality.
Table 1. Bivariate Associations Between Study Variables
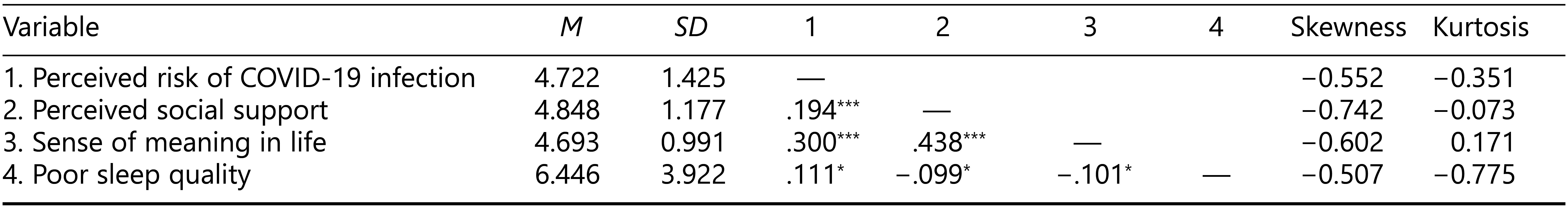
Note. N = 451.
* p < .05. *** p < .001.
The moderated mediation analysis we conducted with PROCESS Model 7 first revealed a significant predictive effect of perceived risk of infection on poor sleep quality, indicating that higher perceived infection risk was associated with worse sleep regardless of other factors (see Table 2). Additionally, there was a significant indirect effect of perceived risk of infection on sleep quality through a diminished sense of meaning in life, but only at low and moderate levels of perceived social support. In other words, participants who felt they had low to moderate social support experienced a stronger negative impact of infection risk on sleep quality because of a reduced sense of meaning in life, whereas this effect was not significant for those with strong social support. In addition, the interaction term between perceived risk of infection and social support significantly predicted a weaker sense of meaning in life.
Table 2. Testing the Moderated Mediation Model
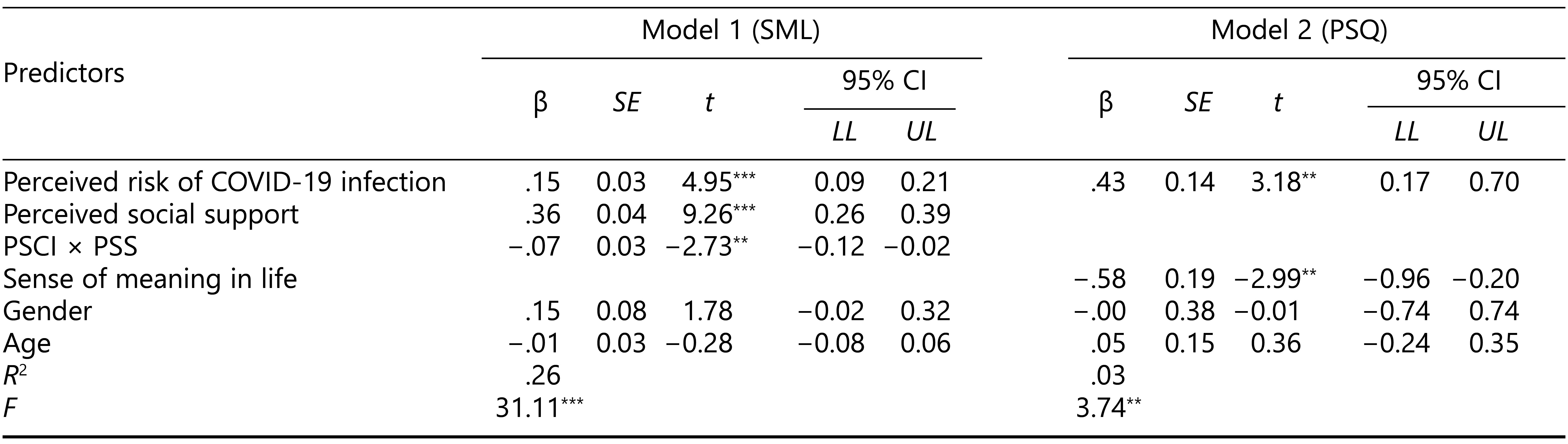
Note. PSCI = perceived risk of COVID-19 infection; PSS = perceived social support; SML = sense of meaning in life; PSQ = poor sleep quality; CI = confidence interval; LL = lower limit; UL = upper limit.
** p < .01. *** p < .001.
A simple slope analysis (see Figure 2) revealed a significant moderating effect of perceived social support on the relationship between perceived risk and sense of meaning in life. Specifically, perceived risk demonstrated a substantially stronger predictive effect on sense of meaning in life among individuals who perceived low levels of social support, β = .23, p < .001, 95% CI [0.16, 0.30], compared to those who perceived high levels of social support, β = .07, p = .142, 95% CI [–0.02, 0.16].
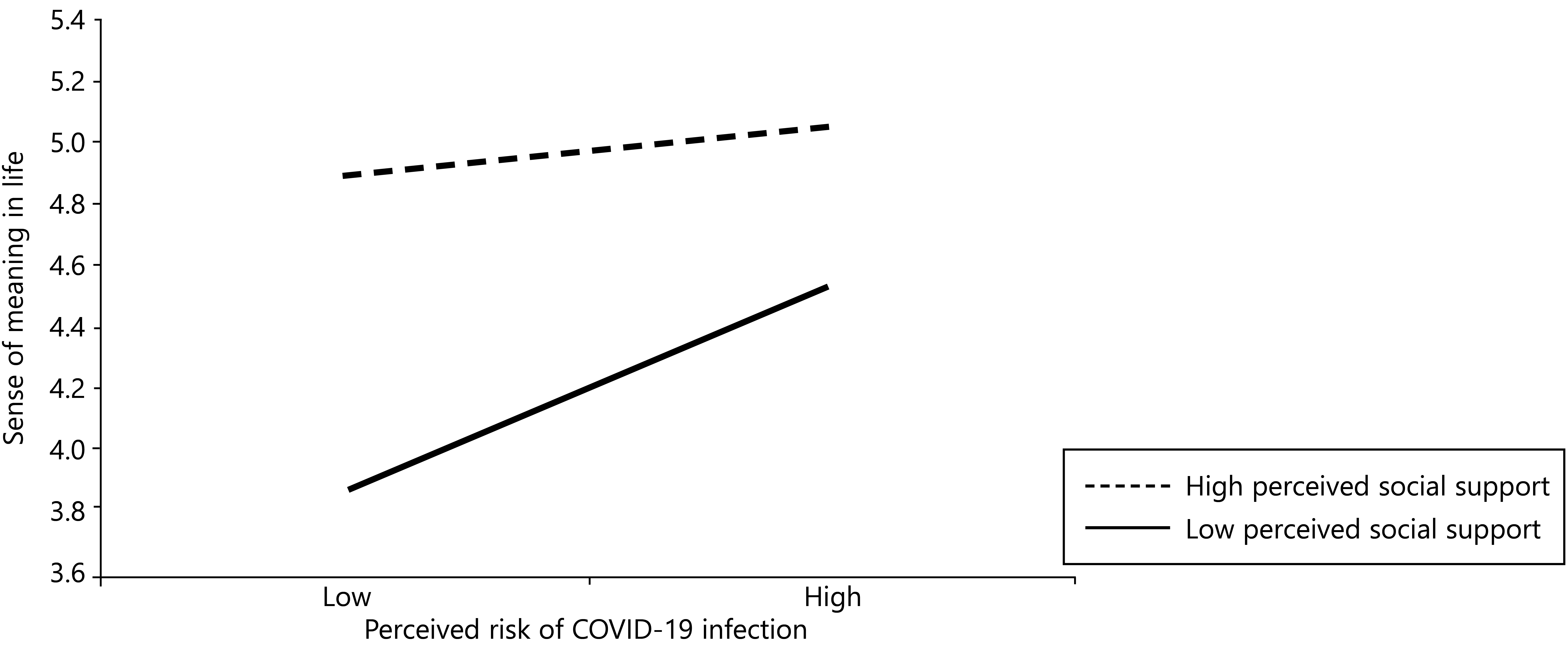
Figure 2. Perceived Risk of COVID-19 Infection and Sense of Meaning in Life as Moderated by Perceived Social Support
Discussion
We investigated the psychological mechanisms underlying the relationship between perceived risk of COVID-19 infection and poor sleep quality. Our findings indicated that perceived risk of COVID-19 significantly predicted poor sleep quality, with sense of meaning in life serving as a partial mediator and perceived social support acting as a moderator.
These results align with those of prior studies showing that individuals who perceive a greater infection risk tend to experience increased sleep disturbances (Lin & Chung, 2021). According to cognitive appraisal theory, individuals’ evaluation of potential threats influences their psychological responses (Folkman et al., 1986); in line with this, we found that perceived risk of infection acted as form of a maladaptive cognitive appraisal that directly undermined sleep quality. This is consistent with earlier experimental research findings, which highlighted the association between threat appraisal and sleep disturbances (Gruenewald et al., 2020). Moreover, our findings supported the strong situation hypothesis (Cooper & Withey, 2009), in which it is suggested that external stressors, such as a pandemic, trigger psychological reactions that are more convergent than are the reactions observed in noncrisis situations. During a public health crisis, the amplified effect of collective anxiety strengthens the pathway through which risk perception impacts sleep quality, leading to psychological vulnerability at the collective level (Zerbini et al., 2022).
Additionally, our results demonstrated that sense of meaning in life partially mediated the relationship between perceived risk of infection and poor sleep quality. Although some researchers have suggested that excessive perceived risk of infection may undermine sense of meaning in life (Shechter et al., 2020), there is also evidence indicating that perceived risk of infection can strengthen individuals’ sense of meaning in life as an adaptive coping strategy (Krok & Zarzycka, 2020). Our findings support the latter perspective, indicating that sense of meaning in life can serve as a psychological resource in a crisis. Furthermore, the negative association between sleep quality and sense of meaning in life that we found aligns with previous research in which a stronger purpose in life (conceptualized as a subset of sense of meaning in life focusing specifically on goal directedness and life orientation) has been linked with better sleep quality, including longer sleep duration and fewer disturbances (Kim et al., 2015). These results highlight the protective role of a sense of meaning in life against sleep disturbances during public health crises (Galek et al., 2015), aligning with the broader construct of meaning as defined in the literature, which may include, but is not limited to, purpose.
We also identified perceived social support as a moderator of the effect of perceived risk of infection on sense of meaning in life, with this effect being significant only in the participants with little (vs. adequate) social support. This finding is consistent with the shock absorber model of social support, which suggests that having robust social networks enhances resilience by promoting positive emotions and buffering the impact of stress (Fu et al., 2022). Individuals with strong social support may experience less anxiety and stress, enabling them to maintain a stable sense of meaning in life despite external threats. In contrast, individuals with little social support may depend more on internal coping mechanisms, making their sense of meaning in life more susceptible to fluctuations based on perceived infection risk, which, in turn, affects their sleep quality.
Theoretical and Practical Implications
This study has extended cognitive appraisal theory by demonstrating that perceived infection risk indirectly influences sleep quality through disrupted meaning-making processes, rather than solely through direct stress pathways. Furthermore, we have provided empirical support for the strong situation hypothesis (Cooper & Withey, 2009) by illustrating how external stressors, such as a pandemic, amplify the psychological effects of risk perception. By identifying social support as a moderator, we have clarified the role of social context in shaping resilience to health threats. Methodologically, this study has advanced previous work by integrating sense of meaning in life (a mediator) and perceived social support (a moderator) into a unified framework, explaining why some individuals maintain resilience despite perceiving a high level of risk, while others experience heightened sleep disturbances.
In terms of practical implications, our findings suggest that the focus in public health interventions should be on fostering a sense of meaning in life (e.g., through meaning-centered interventions or reflective practices) and on strengthening social support networks, especially for vulnerable groups. These dual strategies could help mitigate the negative psychological and sleep-related effects of perceived health risks.
Limitations and Future Research
This study has several limitations. First, our participants exhibited only mild sleep disturbances. Although their scores exceeded the clinical cutoff of ≥ 5, indicating poor sleep quality (Buysse et al., 1989), this is significantly lower than values reported in studies in which the focus was on populations with severe sleep impairments or high-risk groups (e.g., healthcare workers, people with a chronic disease). This may be related to the fact that the study was conducted during the pandemic alleviation period. Compared to the peak of the pandemic, anxiety levels in the population had decreased and the perception of infection risk had weakened, thereby reducing the negative impact of the pandemic on sleep quality (Jahrami et al., 2021). Thus, the conclusions of this study are primarily applicable to the general population with mild sleep problems. Future studies could employ stratified sampling to include groups with varying degrees of sleep disorders and track the dynamic changes in their sleep quality in different phases of a pandemic or public health crisis (Zerbini et al., 2022). Second, the reliance on self-reported online surveys may have introduced social desirability bias. More objective data could be collected to mitigate this bias. Third, the use of a cross-sectional research design precludes the drawing of causal inferences, as individuals with poor sleep quality may also be more likely to perceive higher risk. Future studies could employ longitudinal or experimental designs to establish causality.
Conclusion
In conclusion, this study offers novel insights into the psychological mechanisms linking perceived risk of COVID-19 with poor sleep quality. By identifying sense of meaning in life as a mediator and perceived social support as a moderator, our findings contribute to a deeper understanding of how cognitive and social factors interact to shape sleep health during crises. These insights offer valuable guidance for developing targeted mental health interventions aimed at improving well-being in times of uncertainty.
Alimoradi, Z., Lotfi, A., Lin, C.-Y., Griffiths, M. D., & Pakpour, A. H. (2022). Estimation of behavioral addiction prevalence during COVID-19 pandemic: A systematic review and meta-analysis.
Current Addiction Reports,
9(4), 486–517.
https://doi.org/10.1007/s40429-022-00435-6
Brown, J. K., & Papp, L. M. (2024). COVID‐19 pandemic effects on trajectories of college students’ stress, coping, and sleep quality: A four‐year longitudinal analysis.
Stress & Health,
40(2), Article e3320.
https://doi.org/10.1002/smi.3320
Buysse, D. J., Reynolds, C. F., III, Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research.
Psychiatry Research,
28(2), 193–213.
https://doi.org/10.1016/0165-1781(89)90047-4
Chen, I.-M., Chen, H.-C., Liu, C.-M., Liao, S.-C., Hsieh, M.-H., Wang, T.-Y., Chan, J.-H., & Kuo, P.-H. (2024). The great recession, neurotic personality, and subjective sleep quality among patients with mood disorders.
Humanities and Social Sciences Communications,
11, Article 969.
https://doi.org/10.1057/s41599-024-03467-7
Chen, S., & Cheng, C. (2024). Unveiling coronasomnia: Pandemic stress and sleep problems during the COVID-19 outbreak.
Nature and Science of Sleep,
16, 543–553.
https://doi.org/10.2147/NSS.S459945
Cheung, D. S. T., Yu, B. Y.-M., Lam, S. C., Leung, D. Y. P., Chung, K.-F., Ho, F. Y.-Y., Chen, S.-C., & Yeung, W.-F. (2024). A longitudinal study on the change in sleep across three waves of the COVID-19 outbreaks in Hong Kong.
Sleep and Biological Rhythms,
22(1), 93–102.
https://doi.org/10.1007/s41105-023-00486-w
Faul, F., Erdfelder, E., Lang, A.-G., & Buchner, A. (2007). G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences.
Behavior Research Methods,
39(2), 175–191.
https://doi.org/10.3758/BF03193146
Feeney, B. C., & Collins, N. L. (2015). A new look at social support: A theoretical perspective on thriving through relationships.
Personality and Social Psychology Review,
19(2), 113–147.
https://doi.org/10.1177/1088868314544222
Folkman, S., Lazarus, R. S., Dunkel-Schetter, C., DeLongis, A., & Gruen, R. J. (1986). Dynamics of a stressful encounter: Cognitive appraisal, coping, and encounter outcomes.
Journal of Personality and Social Psychology,
50(5), 992–1003.
https://doi.org/10.1037//0022-3514.50.5.992
Fu, Y.-N., Feng, R., Liu, Q., He, Y., Turel, O., Zhang, S., & He, Q. (2022). Awe and prosocial behavior: The mediating role of presence of meaning in life and the moderating role of perceived social support.
International Journal of Environmental Research and Public Health,
19(11), Article 6466.
https://doi.org/10.3390/ijerph19116466
Galek, K., Flannelly, K. J., Ellison, C. G., Silton, N. R., & Jankowski, K. R. B. (2015). Religion, meaning and purpose, and mental health.
Psychology of Religion and Spirituality,
7(1), 1–12.
https://doi.org/10.1037/a0037887
Gao, C., & Scullin, M. K. (2020). Sleep health early in the coronavirus disease 2019 (COVID-19) outbreak in the United States: Integrating longitudinal, cross-sectional, and retrospective recall data.
Sleep Medicine,
73, 1–10.
https://doi.org/10.1016/j.sleep.2020.06.032
Gruenewald, T., Ong, A., & Zahn, D. (2020). Age variations in perceived COVID-19 threats, negative impacts, and associations with well-being.
Innovation in Aging,
4(Suppl. 1), 933.
https://doi.org/10.1093/geroni/igaa057.3420
Hayes, A. F., & Scharkow, M. (2013). The relative trustworthiness of inferential tests of the indirect effect in statistical mediation analysis: Does method really matter?
Psychological Science,
24(10), 1918–1927.
https://doi.org/10.1177/0956797613480187
Huang, W., Wen, X., Li, Y., & Luo, C. (2024). Association of perceived stress and sleep quality among medical students: The mediating role of anxiety and depression symptoms during COVID-19.
Frontiers in Psychiatry,
15, Article 1272486.
https://doi.org/10.3389/fpsyt.2024.1272486
Jahrami, H., BaHammam, A. S., Bragazzi, N. L., Saif, Z., Faris, M., & Vitiello, M. V. (2021). Sleep problems during the COVID-19 pandemic by population: A systematic review and meta-analysis.
Journal of Clinical Sleep Medicine,
17(2), 299–313.
https://doi.org/10.5664/jcsm.8930
Krok, D., & Zarzycka, B. (2020). Risk perception of COVID-19, meaning-based resources and psychological well-being amongst healthcare personnel: The mediating role of coping.
Journal of Clinical Medicine,
9(10), Article 3225.
https://doi.org/10.3390/jcm9103225
Lin, S.-Y., & Chung, K. K. H. (2021). Risk perception, perception of collective efficacy and sleep quality in Chinese adults during COVID-19 pandemic in Hong Kong: A cross-sectional study.
International Journal of Environmental Research and Public Health,
18(21), Article 11533.
https://doi.org/10.3390/ijerph182111533
Liu, C., Lee, Y.-C., Lin, Y.-L., & Yang, S.-Y. (2021). Factors associated with anxiety and quality of life of the Wuhan populace during the COVID‐19 pandemic.
Stress & Health,
37(5), 887–897.
https://doi.org/10.1002/smi.3040
Lu, H., Yang, J., Zhao, K., Jin, Z., Wen, X., Hu, N., Yang, H., Sun, Z., Chen, H., Huang, Y., Wang, D. B., & Wu, Y. (2024). Perceived risk of COVID-19 hurts mental health: The mediating role of fear of COVID-19 and the moderating role of resilience.
BMC Psychiatry,
24(1), Article 58.
https://doi.org/10.1186/s12888-024-05511-x
Martins, E. L. M., Salamene, L. C., Lucchetti, A. L. G., & Lucchetti, G. (2022). The association of mental health with positive behaviours, attitudes and virtues in community-dwelling older adults: Results of a population-based study.
International Journal of Social Psychiatry,
68(2), 392–402.
https://doi.org/10.1177/0020764021999690
Park, C. L. (2010). Making sense of the meaning literature: An integrative review of meaning making and its effects on adjustment to stressful life events.
Psychological Bulletin,
136(2), 257–301.
https://doi.org/10.1037/a0018301
Shechter, A., Diaz, F., Moise, N., Anstey, D. E., Ye, S., Agarwal, S., Birk, J. L., Brodie, D., Cannone, D. E., Chang, B., Claassen, J., Cornelius, T., Derby, L., Dong, M., Givens, R. C., Hochman, B., Homma, S., Kronish, I. M., Lee, S. A. J., . . . Abdalla, M. (2020). Psychological distress, coping behaviors, and preferences for support among New York healthcare workers during the COVID-19 pandemic.
General Hospital Psychiatry,
66, 1–8.
https://doi.org/10.1016/j.genhosppsych.2020.06.007
Steger, M. F., Frazier, P., Oishi, S., & Kaler, M. (2006). The Meaning in Life Questionnaire: Assessing the presence of and search for meaning in life.
Journal of Counseling Psychology,
53(1), 80–93.
https://doi.org/10.1037/0022-0167.53.1.80
Steger, M. F., Oishi, S., & Kashdan, T. B. (2009). Meaning in life across the life span: Levels and correlates of meaning in life from emerging adulthood to older adulthood.
The Journal of Positive Psychology,
4(1), 43–52.
https://doi.org/10.1080/17439760802303127
Svenson, O., Isohanni, F., Salo, I., & Lindholm, T. (2024). Airborne SARS-CoV2 virus exposure, interpersonal distance, face mask and perceived risk of infection.
Scientific Reports,
14(1), Article 2285.
https://doi.org/10.1038/s41598-024-52711-2
Wang, Y., Wan, Q., Huang, Z., Huang, L., & Kong, F. (2017). Psychometric properties of Multi-Dimensional Scale of Perceived Social Support in Chinese parents of children with cerebral palsy.
Frontiers in Psychology,
8, Article 2020.
https://doi.org/10.3389/fpsyg.2017.02020
West, S. G., Finch, J. F., & Curran, P. J. (1995). Structural equation models with nonnormal variables: Problems and remedies. In R. H. Hoyle (Ed.), Structural equation modeling: Concepts, issues, and applications (pp. 56–75). Sage Publications, Inc.
Wismans, A., van der Zwan, P., Wennberg, K., Franken, I., Mukerjee, J., Baptista, R., Marín, J. B., Burke, A., Dejardin, M., Janssen, F., Letina, S., Millán, J. M., Santarelli, E., Torrès, O., & Thurik, R. (2022). Face mask use during the COVID-19 pandemic: How risk perception, experience with COVID-19, and attitude towards government interact with country-wide policy stringency.
BMC Public Health,
22(1), Article 1622.
https://doi.org/10.1186/s12889-022-13632-9
Wolfson, J. A., Garcia, T., & Leung, C. W. (2021). Food insecurity is associated with depression, anxiety, and stress: Evidence from the early days of the COVID-19 pandemic in the United States.
Health Equity,
5(1), 64–71.
https://doi.org/10.1089/heq.2020.0059
Zerbini, G., Taflinger, S., Reicherts, P., Kunz, M., & Sattler, S. (2022). Perceived risk of COVID‐19 exposure and poor COVID‐19 prognosis impair sleep: The mediating and moderating roles of COVID‐19‐related anxiety and knowledge.
Journal of Sleep Research,
31(5), Article e13569.
https://doi.org/10.1111/jsr.13569
Zhang, K., Zhang, N., Wang, J., Jiang, J., & Xu, S. (2022). Exploring the roles of fear and powerlessness in the relationship between perceived risk of the COVID-19 pandemic and information-avoidance behavior.
Frontiers in Psychology,
13, Article 1005142.
https://doi.org/10.3389/fpsyg.2022.1005142
Zimet, G. D., Dahlem, N. W., Zimet, S. G., & Farley, G. K. (1988). The Multidimensional Scale of Perceived Social Support.
Journal of Personality Assessment,
52(1), 30–41.
https://doi.org/10.1207/s15327752jpa5201_2







